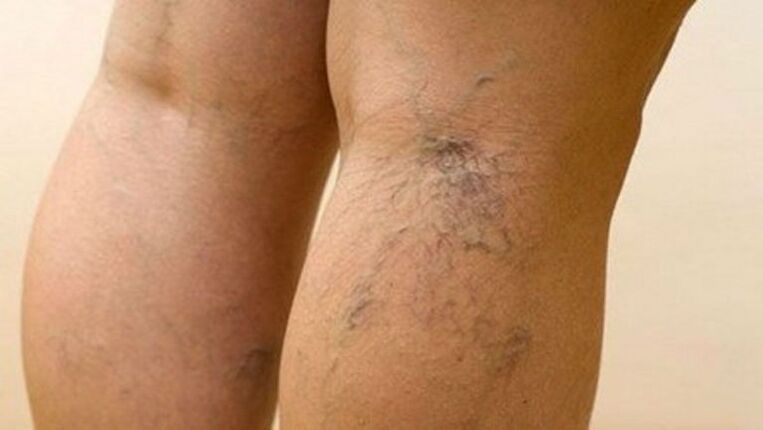
Varicose veins of the lower extremities, according to information on appeal to medical institutions, is found in every fifth man and 28% of women of working age.
If we consider the entire population, then half of adults will have characteristic symptoms.
The peculiarity of this disease is growth from comfortable living conditions. Studies in Asian countries have shown a lower prevalence among the poor who are engaged in manual labor, making long walks.
Why are the veins of the legs loaded?
The anatomical structure of the vein wall is characterized by a reinforced skeleton of muscles and a valve apparatus. The expediency lies in the need not only to keep the blood flow in the vertical position of a person, but also to organize its rise against gravity in the direction towards the heart.
The valves block the return flow to prevent overfilling at the most distant points of the body. This "uncomfortable" place is the legs and feet.
The mechanism of formation of varicose veins of the legs
At the age of 40, the human body begins to synthesize limitedly plastic materials, the main of which is the collagen protein. It is essential for good venous valve tone. The absence leads to loss of tone, sagging and inability to delay the reverse flow of blood and the overlying mass.
The venous network in the legs consists of superficial vessels lying directly under the skin and deep veins located in the thickness of the muscle layer.
Varicose veins of the lower extremities are characterized by an initial lesion of the valves of the superficial veins. Congestion manifests itself in areas with dilated fine veins, visible to the eye in the form of a fine mesh.
Further development of the pathology leads to blood retention in the periphery and causes tissue edema (fluid escape through the walls of the veins), malnutrition (the outflow of toxins is reduced, oxygen and nutrients are retained by squeezed arteries).
How complications join
Stagnation of venous blood in the legs causes a slowed down blood flow in the vessels, and this creates favorable conditions for the aggregation (gluing) of platelets. Blood clots complicate an already compromised blood supply.
The risk of embolus rupture and its movement through large vessels to the heart increases. If a person has defects associated with the communication of the right and left chambers, it is possible for an embolus to enter the arterial blood and the development of necrotic changes in the organs.
The most common concomitant complication is the addition of a local infection in the affected area of the venous wall, followed by the development of phlebitis or thrombophlebitis.
Causes of the disease
For varicose veins of the lower extremities, there is only one reason independent of a person - a genetic deficiency in the structure of collagen. It manifests itself not only in varicose veins, but also in relatively early signs of skin aging (dryness, deep wrinkles).
Other reasons are related to the activities and behavior of people.
- Decreased physical activity or, conversely, hard physical labor leads to a violation of the tone of the veins of the legs.
- Prolonged forced standing, sitting during working hours causes stagnation of blood in the legs and impaired outflow.
- Pregnancy puts increased pressure on the pelvic organs and large veins, preventing drainage from the lower veins.
- Doctors from Asian countries associate the growth of leg varicose veins in patients with an addiction to the European habit of sitting in a chair or on a chair instead of bent knees.
- Comfortable high toilets require increased tension of the muscles of the abdominal wall during bowel movements, straining contributes to stagnation in the legs. While squatting, the act of defecation is more physiological.
- The habit of fast food, a decrease in the proportion of raw vegetables and fruits in the diet lead to constipation and prolonged stress.
- Smokers expose the entire body to nicotine, which acts on the veins as a paralyzing poison.
- Fashionable high-heeled footwear leads to improper stress on the leg muscles and disrupts the tone of the veins.
- Common pills, hormonal contraceptives, treatment with hormonal drugs for menopause, osteoporosis lead to impaired collagen synthesis.
- The advertised slimming underwear and the wearing of tight jeans cause blood to stagnate in the underlying parts of the body.
Who should be included in the risk group
Considering the listed reasons for the development of venous pathology, the group of persons with an increased likelihood of developing varicose veins of the legs should include:
- people professionally associated with a long stay in a standing or sitting position (salespeople, teachers, hairdressers, drivers, office workers);
- women who prefer skinny jeans, shaping underwear and high-heeled shoes;
- people involved in weightlifting and bodybuilding;
- people who are accustomed to sitting "side to side";
- women with frequent pregnancies and childbirth, as well as taking hormonal contraceptives;
- smokers, lovers of strong coffee and alcohol;
- constipated.
Preventive measures are needed for these populations.
Symptoms
The first symptoms of varicose veins in the legs are noticeable at a young age. In the initial stage, they appear with increased load on the legs:
- by the end of the shift, pains appear in the feet and legs, muscle fatigue;
- when changing shoes, swelling of the feet is found due to the tightness of the shoes;
- in the evening the feet "burn", you want to dip them into cold water;
- "spiders" are formed on the skin of the thighs and legs.

At the next stage, a picture of chronic venous insufficiency develops, symptoms of internal varicose veins appear:
- disturbed by night cramps in the calves, cramps when walking are possible;
- dark spots, dryness, peeling appear on the skin of the feet and legs;
- the appearance of trophic ulcers, very painful, with loose edges, difficult to treat.
If, against the background of local pain, swelling, redness of the skin, an increase in body temperature are found, you need to think about thrombophlebitis.
Diagnostics
In diagnostics, it is customary to distinguish between true (primary) varicose veins, depending on the lesion of the valve apparatus, and secondary, resulting from trauma and tumors.
Surgeons of polyclinics, vascular surgeons, phlebologists are involved in the examination. The doctor sees subcutaneous venous nodes, vascular networks, skin pigmentation, beginning ulcers, dermatitis.
On palpation, the tension of the superficial veins, the density of the wall, the size of local changes, the presence of a thrombus, the temperature of the skin over the nodes (signs of thrombophlebitis) are assessed.
A general blood test will show the onset of inflammation (leukocytosis, accelerated ESR), a tendency to thrombus formation according to a coagulogram.
Vascular ultrasound allows you to trace blood flow, function of venous valves, and detect blood clots.
Doppler examination allows you to check the structure of the veins, to make a diagnosis at the initial stage of the disease.
The spiral computed tomography method is carried out in case of difficulties in diagnosis. It makes it possible to obtain a three-dimensional image of the anatomical region, and helps in the choice of surgical treatment.
Treatment of varicose veins of the legs
It is better to start treatment of varicose veins of the legs at the initial stage. To do this, you will have to think about the necessary changes in habits, nutrition, and movement.
Mode
In order not to bring the legs to swelling by the end of the working day, people of "sedentary" and "standing professions" are advised to carry out physical culture breaks or warm-ups with foot massage in an elevated position. Drivers, office workers should walk around during breaks.
The simplest exercises can be done at work:
- barefoot on the floor alternately stand on toes and heels;
- sitting on a chair, raise your legs and make circles with your feet in one direction, then in the other.
Morning exercises should include exercises in a lying position: alternate leg raises, "bicycles", shaking raised legs. Exercises with squats, bent knees are not suitable.
Lovers of strength training should refuse them. Most shown are swimming, cycling, and hiking.
Selection of a balanced diet
Limit all foods that increase weight, promote fluid retention, and increase blood viscosity.
Fatty meat and dairy products, spicy and salty foods, canned food, sweets, baked goods, carbonated drinks are not recommended.
In the daily diet, you should use more vegetables and fruits, berries, onions, garlic, fermented milk products, cereals, vegetable oil is shown instead of butter, walnuts.
Vein support methods
Wearing compression stockings or golf is recommended to support blood flow. They are sized to be worn while lying on your back.
Silicon-filled treads are touted as a remedy that creates an electrical charge on the surface of the foot.
Specialists pay attention to the possible impact of these aids only in the initial stage of the disease. In the presence of superficial nodes and edema on the legs, their use is completely useless.
The use of medicines
Drug treatment consists in the intake of drugs from the group of "venotonic" in a therapeutic dose, selected by the doctor. They help relieve fatigue, discomfort in the feet, but they do not eliminate the disease.

Surgeons attribute medications for varicose veins to the background conservative treatment, but the main one is one of the less traumatic ways of influencing the affected veins. Efficacy is confirmed in 95% of patients. More serious interventions are used only in 5% of patients.
What concerns low-traumatic operations
Low-traumatic methods of treating varicose veins allow you to avoid surgery, rightfully rank first in terms of effectiveness. They do not require a skin incision, can be performed in a polyclinic, and are practically painless. The patient is not limited in terms of work, movement. A long recovery period is not required after surgery.
Laser ablation method
It is performed under local anesthesia. An optical fiber is inserted into the varicose vein, and a circular laser beam is switched on during the reverse movement.
Method action: the beam causes a pronounced burn of the inner lining of the vein, further hardening. The duration of the intervention is about two hours. The method is applicable in the treatment of veins of any size.
Sclerotherapy technique
A substance is injected into the affected vein that can cause the walls to collapse with subsequent scarring. Foam preparations are especially recommended, which quickly and safely fill the lumen of the diseased vein. The method is applicable when the diameter of the vessel is up to 1 cm. After the introduction, it is necessary to walk for an hour. Phlebologists recommend wearing compression socks for another month.
Method of microflebectomy
Under local anesthesia, an incision is made in the skin of several mm, through which a diseased vein is grasped by a hook, brought to the surface of the skin and excised. The method is suitable for venous nodes of any size and diameter. A small scar will remain at the incision site. You must wear compression socks or stockings for 10 days.
Radiofrequency ablation method
It is carried out similarly to laser, but differs in the effect of microwave radio frequencies. This method does not cause tissue burns, therefore it is less traumatic than laser. After 30 minutes of exposure to microwaves, the vessel lumen is sealed. After 7 days, the rehabilitation is considered complete. You can play sports.
In what cases is the operation indicated?
With unsuccessful treatment by conservative methods and the impossibility of using minimally invasive techniques, a phlebectomy operation is prescribed. It allows you to remove large areas of varicose veins, bundles.
The patient is hospitalized. Surgical treatment is performed under general anesthesia. Usually two incisions are made: in the groin area and under the knee. The vein is tied on both sides, pulled outward and removed. Sutures are applied to the incisions. The patient is treated in a hospital for a week. Drugs that reduce blood clotting are used. The stitches are removed after at least 7 days.
Phlebectomy is not performed:
- in the old age of the patient;
- with massive damage to deep and superficial veins;
- during pregnancy;
- with atherosclerosis of the vessels of the legs, diabetes mellitus;
- if there are skin diseases at the site of the proposed operation.

Prevention methods
Prevention of varicose veins of the legs is primarily necessary for people with risk factors in the profession.
It is recommended to walk more. There is a massage and strengthening of the walls of the veins.
During breaks, sellers and hairdressers are shown foot and shin massage. It is done with slow, smooth movements in the direction from the fingers to the knee and along the thigh. The knuckles of the fist are massaged in a circular motion to the central fossa of the foot.
Drivers need to get out of the car, walk around, stretch their legs. Exercises for the legs are shown.
Fashionistas should think about the consequences before getting into high heels and wearing tight clothes.
At home, you can do contrast baths or foot showers. Apply a compress on tired legs with decoctions of chamomile, chestnut, wormwood, burdock.
A timely visit to the surgeon allows you to get rid of painful problems, restore activity and movement.



































